මැලේරියාව
මෙම ලිපිය සත්යාපනය සඳහා තවත් අමතර මූලාශ්ර දැක්වීම කළ යුතුව ඇත. |
| මැලේරියාව | |
|---|---|
| වර්ගීකරණය සහ බාහිර මූලාශ්ර | |
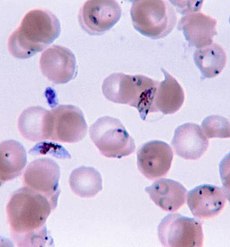 ප්ලැස්මෝඩියම් ෆැල්සිපැරම් වළලුමය-ව්යුහ සහ මිනිස් රුධිරයෙහි ජන්මාණුසෛලයන්. | |
| ICD-10 කේතය | B50. |
| ICD-9 කේතය | 084 |
| OMIM | 248310 |
| DiseasesDB | 7728 |
| MedlinePlus | 000621 |
| eMedicine | med/1385 emerg/305 ped/1357 |
| MeSH | C03.752.250.552 |
මැලේරියාව යනු වාහකයෙක් මගින් බෝවන ආසාදිත රෝගයක් වන අතර එය ඇති කරනු ලබන්නේ ප්රොටෝසෝවාවකු (ඒක සෛලික ජීවියෙක්) වූ පරපොෂිතයෙකුගෙනි. එය ඇමරිකාව , ආසියාව සහ අප්රිකාව වැනි නිවර්තන සහ උපනිවර්තන ප්රදේශවල වඩාත් පුළුල්ව පැතිර පවතී. සෑම වසරක් තුළම එමගින් මිලියන 515 ක් තරම් ජනතාව රෝගී කරන අතර මිලියන 1 සිට 3 අතර රෝගීන් ප්රමාණයක් මරණයට පත්කරනු ලබයි. මේ අතරින් බහුතරයක් වනුයේ උපසහරා අප්රිකාවෙහි ජීවත් වන කුඩා ළමුන්ය. මැලේරියාව බහුල වශයෙන් දිළිදු බව සමග අනුබද්ධව පැවතුන ද එය දිලිදුකම සහ ආර්ථික වර්ධනයට ඇති බාධාවලට හේතුවක් ලෙස ද ඇති වේ.
මැලේරියාව බහුලවම ඇති බෝවන රෝග වලින් එකක්වන අතර එය දැඩි මහජන සෞඛ්ය ගැටළුවකි. මෙම රෝගය ඇති කරනු ලබන්නේ ප්ලැස්මෝඩියම් ගණයට අයත් ඒක සෛලික පරපොෂිතයෙක් මගිණි. මිනිසුන් හට ආසාදන ඇති කළ හැක්කේ මෙම ප්ලැස්මෝඩියම් වර්ගයට අයත් පරපෝෂිතයන් 4 දෙනෙකුගෙන් පමණි. වඩාත් දරුණු මැලේරියා රෝග තත්වයන් ඇති කරනු ලබන්නේ ප්ලැස්මෝඩියම් ෆල්සිපාරුම් හා ප්ලැස්මෝඩියම් වයිවැක්ස් නම් පරපෝෂිතයන්ගෙනි. නමුත් අනෙකුත් වර්ග දෙක වන ප්ලැස්මෝඩියම් ඕවාලේ සහ ප්ලැස්මෝඩියම් මලාරියේ යන පරපෝෂිතයින්ට ද මිනිසුන් හට ආසාදන ඇති කිරීමේ හැකියාව ඇත. මෙම මිනිසුන් සදහා රෝග ඇති කරන ප්ලැස්මෝඩියම් විශේෂවලට මැලේරියා පරපෝෂිතයින් ලෙස සාමාන්ය වහරයේදී හැදින්වේ.
මැලේරියා පරපෝෂිතයින් පරිවහණය කරනු ලබන්නේ ගැහැණු ඇනෝපිලස් මදුරුවකු මගිණි. මෙම පරපෝෂිතයින් මිනිසාගේ රුධිරයෙහි වූ රක්තානුවල ගුණනය වීමෙන් රෝග ලක්ෂණ ඇති කරනු ලබයි. ඒවා නම් රක්ත හීනතාවයෙහි රෝග ලක්ෂණ, (හිසෙහි ඇති වන සැහැල්ලු බව, හුස්ම ගැනීමේ අපහසුතාව, හෘද ස්පන්ධනය ඉහළයෑම ....) උණ , ඇග සීතල වීම, ඔක්කාරය සහ රෝගය වඩාත් දරුණු අවස්ථාවන්හිදී කෝමා තත්වය සහ මරණය පවා ඇති වේ. මැලේරියා රෝගය ව්යාප්ත වීම මදුරුදැල් සහ කෘමිවිකර්ශක ද්රව්ය භාවිතා කර ගැනීමෙන් මදුරුවන් ලවා දෂ්ටවීම වළක්වා ගැනීම මගින් අවම කර ගත හැකිය. කෘමිනාශක වර්ග ඉසීම හා මදුරුවන් බිත්තර දමන ජලය එකතු වන තැන් ඉවත් කිරීම මගින් ඔවුන් බෝවීම පාලනය කළ හැකිය.
ඇතැම් එන්නත් වර්ග පර්යේෂණ මට්ටමෙන් පැවතුනද මේ වන විට මැලේරියාවට එරෙහි එන්නතක් සොයා ගෙන නොමැත. රෝගය ඇති වීම සදහා ඇති අවධානම අඩුකරගැනීම සදහා රෝග වළක්වා ගැනීමේ ඖෂධ වර්ග නොකඩවා භාවිතා කළ යුතු වේ. රෝගය බහුලවම පවතින ප්රදේශ වල ජීවත් වන ජනතාව සදහා මෙලෙස රෝග වළක්වා ගැනීම සදහා ඖෂධ භාවිතා කිරීම ඇතැම් අවස්ථාවලදී අපහසු වන්නේ ඒවා මිල අධික බැවිණි. රෝගය බහුලව පවතින ප්රදේශවල සිටින වැඩිහිටියන් බොහොමයකට දිගු කාලීනව වරින් වර රෝගය ඇති වන අතර ඔවුන් රෝගය සදහා අසම්පුර්ණ වශයෙන් ප්රතිරෝධීතාවයක් දක්වති. නමුත් ඔවුන් මැලේරියාව නොමැති ප්රදේශයක සැලකිය යුතු තරම් කාලයක් ගත කළහොත් මෙම ප්රතිරෝධතාවය අඩුවන අතර එවන් පුද්ගලයින් මාරාන්තික මැලේරියා රෝගී තත්වයන් සදහා ගොදුරු වීමට ද හැකියාව පවතී. එමනිසා එම පුද්ගලයින් මැලේරියා රෝගය පවතින ප්රදේශයකට ඇතුළු වන විට සම්පූර්ණ වශයෙන් ආරක්ෂක ක්රමෝපායන් භාවිතා කිරීමට තදින්ම අවවාද කෙරේ. ඖෂධ සදහා ඇති ප්රතිරෝධීතාවය වඩාත් බහුලවම දක්නට ඇතත් මැලේරියා ආසාදන ක්වීනින් හා ආටිමිස්නීන් ව්යුත්පන්න යන ප්රතිමැලේරියා ඖෂධ යොදා ගෙන ප්රතිකාර කරනු ලබයි.
ඉතිහාසය
[සංස්කරණය]වසර 50000 කටත් වැඩි කාලයක් මුළුල්ලේ මැලේරියා රෝගය මගින් පුද්ගලයන් ආසාදයට ලක්කර ඇති අතර මුළු ඉතිහාසය පුරාවටම එය මිනිසුන් සදහා ආසාදන ඇති කරන ව්යාධි ජනකයෙකු ලෙස හදුනාගෙන ඇත. මානව මැලේරියා පරපෝෂිතයින්ගේ සමීප ඥාතීන් මානවයන්ගේ සමීපතම ඥාතීන් වන චින්පන්සීන්ගේ ද දක්නට ඇත. බුද්ධ වර්ෂ 2700 යෙහි මුල භාගයේ දී චීනයේ ද මැලේරියාව මගින් ඇති කරන එයටම අාවේනික වූ කාලාවර්තන උණ ඇති කිරීමක් (Periodic Fever) පිළිබදව වාර්තා වී ඇත. මැලේරියා යන වචනය සම්භවය වී ඇත්තේ ඉතාලි භාෂාවෙන් “අහිත කර වාතය” යන තේරුම ඇතිවය. මැලේරියා රෝගය වගුරු බිම් ආශ්රිතව ඇති වන්නක් නිසා මුල් අවධිවලදී එය ගැහෙන උණ හෝ වගුරු උණ යයි හදුන්වන ලදී.
1880 වේදී මැලේරියාව පිළිබදව සිදු කරන ලද විද්යාත්මක අධ්යයනයන් ඒවායෙහි මුල්ම කැපී පෙනෙන වෙනස් කම් පෙන්නුම් කරන ලදී. චාල්ස් ලුවී අල්පොන්සෝ ලාවේරාන් නම් ඇල්ජීරියාවෙහි හමුදා රෝහලක සේවය කළ ප්රංශ ජාතික හමුදා වෛද්යවරයෙකු විසින් මැලේරියා රෝගයෙන් පීඩා විදින පුද්ගලයෙකුගේ රතු රුධිර සෛල තුළ වූ මැලේරියා පරපෝෂිතයින් මුල්වරට නිරීක්ෂණය කිරීමත් සමගම ඉහත සදහන් කරන ලද වෙනස් කම් සිදුවුණි. මුල්වරට ඒක සෛලික පරපෝෂිතයෙකු මගින් රෝග ඇති කළ හැකි බවට සොයා ගනිමින් ඔහු විසින් හදුනා ගන්නා ලද මෙම ඒක සෛලික ජීවින් විසින් මැලේරියාව ඇති කරන බවට ඔහු යෝජනා කරන ලදී. ඔහු විසින් සිදු කරන ලද මෙම සොයා ගැනීම සහ පසුකාලීනව සිදු කරන ලද සොයා ගැනීම් සම්බන්ධයෙන් 1907 දී වෛද්ය විද්යාව සදහා වූ නොබෙල් ත්යාගය හිමිකර ගන්නා ලදී. මෙම ඒක සෛලික ජීවින් හට ඉතාලි ජාතික විද්යාඥයන් දෙපලක් වූ Ettore Marchiafava සහ Angelo Celli විසින් ප්ලැස් මෝඩියම් ලෙස නම් කරන ලදී. මින් පසු වර්ෂයකදී හවානාහි කහ උණ සහිත රෝගීන් හට ප්රතිකාර කරන කියුබානු වෛද්යවරයෙකු වූ කාලෝස් ෆිනාලෝ විසින් මදුරුවන් මගින් මිනිසාට සහ මිනිසාගෙන් පිටතට රෝග ව්යාප්ත කළ හැකි බවට සොයා ගන්නා ලදී. කෙසේ නමුත් ඉන්දියාවෙහි සේවය කරන ලද බ්රිතාන්ය ජාතික වෛද්යවරයෙකු වූ සර් රොනාල්ඩ් රෝස් විසින් අවසන් වරට 1898 දී ඔප්පු කරන ලද්දේ මැලේරියාව මදුරුවන් මගින් පරිවහනය වන බවයි. ඔහු මෙය සිදුකරන ලද්දේ ඇතැම් මදුරු විශේෂ මගින් මැලේරියා රෝගය ව්යාප්ත කරන බව පෙන්වීම මගින් සහ ආසාදිත පක්ෂීන්ගෙන් ලේ උරා බොන ලද මදුරුවන්ගේ ඛේට ග්රන්ථිවලින් මැලේරියා පරපෝෂිතයින් වෙන්කිරීම මගිනි. ඔහුගේ මෙම සොයා ගැනීම සදහා 1902 දී වෛද්ය විද්යාව සදහා වූ නොබෙල් ත්යාගය ඔහුට හිමිවුණි. ඉන්දියානු වෛද්ය සේවයෙන් විශ්රාම ගැනීමත් සමගම රෝස් අළුතෙන් ස්ථාපිත කරන ලද නිවර්තන රටවල වෛද්ය විද්යාව පිළිබදව වූ ලිවර්පූල් පාසලෙහි සේවයට බැදුනු අතර එමගින් ඊජිප්තුව , පැනමාව, ග්රීසිය සහ මුරුසිය යන රටවල මැලේරියාව පාලනය සදහා ක්රියාකරන ලදී. ෆින්ලේ සහ රෝස් විසින් කරන ලද සොයා ගැනීම් 1900 දී වොල්ටර් රිඩ්ගේ මූලිකත්වයෙන් පැවති වෛද්ය මඩුල්ලක් මගින් සම්මත කරන ලද අතර එමගින් කරන ලද අනුමත කිරීම් ක්රියාවට නංවන ලද්දේ පැනමා ඇල ගොඩ නගන කාලසීමාවේදී විලියම් සී ගෝගාස් විසින් සිදුකරන ලද සෞඛ්ය වැඩසටහන් වලදීය. මෙම මහජන සෞඛ්ය ක්රියාකාරකම් මගින් දහස් ගණනක් වූ සේවකයන්ගේ ජීවිත බේරා ගැනීමට හැකියාව ලැබුණු අතර රෝගයට එරෙහිව අනාගතයේ දී මහජන සෞඛ්ය ව්යාපාර ඇති කිරීම සදහා ක්රමෝපායන් ගොඩ නැගීමට ද එමගින් උපකාර වුණි.
මැලේරියා රෝගය සදහා මුල්ම ඵලදායි ප්රතිකාර ක්රමය වූයේ ක්වීනීන් අන්තර්ගත සින්කෝනා ශාකයේ පොත්තයි. මෙම ශාකය ප්රධාන වශයෙන් පීරූ රාජ්යයෙහි ඇන්දීස් නම් කදු ගැටයෙහි බෑවුම්වල වර්ධනය වේ. පීරූ රාජ්යයෙහි වාසය කරන්නන් විසින් මෙම ස්වාභාවික නිෂ්පාදනය මැලේරියා රෝගය පාලනය සදහා භාවිතා කරන ලද අතර රෝමාණු කතෝලික සභාව විසින් 1640 දී මෙය යුරෝපයට හදුන්වා දෙන ලද අතර එහිදී එය ඉතා සීඝ්රයෙන් පිළිගැනීමට ලක්වුණි. කෙසේ නමුත් 1820 දී ප්රංශ ජාතික රසායනික විද්යාඥයන් දෙදෙනෙකු වන Pierre Joseph Pelletier සහ Joseph Bienaime Caventou විසින් සිංකෝනා ශාකයේ පොත්තෙන් සක්රීය අන්තර්ගතය නිස්සාරණය කරගෙන එය ක්වීනින් ලෙස නම් කරන ලදී.
විසිවන සියවසෙහි මුල්භාගයේදී ප්රතිජීවක ඖෂධ සොයා ගැනීමටත් ප්රථම උපදංශය සහිත රෝගීන් හිතාමතාම මැලේරියා රෝගය මගින් ආසාදනයට ලක්කර උණ ඇති කරන ලද අතර මෙම ක්රියාකාර කම් සිදුකිරීමට පුරෝගාමි වුයේ Julius Wagner Jauregg ය. නමුත් ක්විනීන් භාවිතයෙන් නිරවද්යව උණ පාලනය කිරීමත් සමගම උපදංශය සහ මැලේරියාව මගින් ඇතිවන ප්රතිඵල අවමකරගත හැකි වුණි. ඇතැම් රෝගීන් මැලේරියාව නිසා මරණයට පත් වුවද එය උපදංශය නිසා ඇති වු ඇතැම් මරණ වලට වඩා වැඩි අවධානයක් යොමුකර ගත්තේය.
මැලේරියා ජීවන චක්රයෙහි රුධිරය තුල සහ මදුරුවා තුල ඇති අවධි දහනව වන සහ විසිවන සියවසෙහි මුල්බාගයේදී හදුනා ගත්තද 1980 වන තෙක්ම මිනිසාගේ අක්මාව තුල අප්රකටව සැගවී පවත්නා පරපෝෂිත අවධිය හදුනාගෙන නොතිබිණි. මෙම අප්රකට පරපෝෂිත අවධිය හදැනාගැනීමත් සමගම ඇතැම් රෝගීන් මැලේරියා පරපෝෂිතයෙන් ඔවුන්ගේ රුධිරයෙන් සම්පුර්ණයෙන්ම අතුරුදන් වී රෝගය සුව වීමෙන් පසුවද වසර ගනාවකට පසු නැවත රෝගය හටගැනීමට හේතුව සොයා ගන්නා ලදී.
නූතන වෛද්ය විද්යාව සහ එහි ප්රායෝගික කරණයේදී විෂබීජ නාශකවල සිට එන්නත් වර්ග සහ ප්රතිජීවක ඖෂධ දක්වා විවිධ වශයෙන් දිවෙන ඵලදායී උපකරණ හා ආම්පන්න සමුදායක් පවතී. අතීතයේදී වෛද්ය විද්යාව ඉතා දුර්වලව පැවති එක් ක්ෂේත්රයක් වූයේ වෛරස ආසාදනවලට එරෙහිව ක්රියා කළ හැකි ඖෂධයක් සොයාගැනීම සම්බන්ධවය. නූතනයේදී එවන් වෛරස ආසාදනවලින් ඇතිවන රෝග වළක්වා ගැනීම සදහා ඉතාමත් ඵලදායී එන්නත් වර්ග සොයා ගෙන ඇත. නමුත් ඊට පෙර අවධිවල දී යම් කිසි පුද්ගලයෙකුට වෛරස ආසාදනයක් ඇති වුවහොත් ඒ සදහා කිසිදු ක්රියාමාර්ගයක් ගැනීමට හැකියාව නොතිබූ අතර එම රෝගීන් සදහා අනුමත කරන ලද්දේ අදාල රෝගය ස්වාභාවිකවම සුවපත් වන තෙක්ම ප්රමාණවත් තරම් විවේක ගැනීම සහ දියර වර්ග පානයට ලබාදීමයි.
ප්රථම වරට පරේක්ෂණාත්මක මට්ටමේ ප්රතිවෛරස ඖෂධය නිෂ්පාදනය කරන ලද්දේ 1960 දී වන අතර එමගින් හර්පීස් වෛරසයට එරෙහිව ක්රියාකිරීමේ හැකියාව ලැබුණි. මෙම ඖෂධ වර්ග සොයා ගන්නා ලද්දේ සාම්ප්රදායිකව සිදු කරන ලද පිරික්සුම් හා වැරදීම් න්යාය මත පදනම්ව ඖෂධ වර්ග සොයා ගැනීෙම් ක්රමෝපායන් මතයි. ඔවුන් ඉන්පසුව මෙලෙස සොයා ගන්නා ලද රසායනික ද්රව්යය වෛරස වර්ධනය කරන වර්ධක මාධ්යයක් වෙතට හදුන්වා දුන් අතර ඔවුන් විශ්වාස කළේ ඒවා මගින් වෛරසවල ක්රියාකාරිත්වය අත්හිටුවිය හැකිබවයි. එබැවින් ඉන්පසු ඔවුන් එම වර්ධක මාධ්යය තුළ අදාල වෛරසය වර්ධනය වීමක් හෝ වර්ධනය අඩාල වීමක් ඇති වේදැයි නිරීක්ෂණය කරන ලදී. මෙලෙස ඵලදායි ප්රතිඵල ලබාදුන් රසායනික ද්රව්යය තව දුරටත් සමීප වශයෙන් අධ්යයනය කිරීම සදහා තෝරා ගන්නා ලදී.
මෙය බොහෝ කාලයක් තිස්සේ කාලය මිඩංගු කරමින් සිදුකළ ක්රියා පටිපාටියක් වන අතර ඉලක්ක කරන ලද වෛරසයෙහි ක්රියාකාරිත්වය පිළිබදව හොද දැනීමක් නොමැතිව ඵලදායි සහ අතුරු ආබාධ අවම ප්රතිවෛරස ඖෂධ නිෂ්පාදනය කිරීමට හැකියාවක් නොලැබුණි. 1980 වේදී වෛරසවල සම්පුර්ණ ජාන අනුපිලිවෙල හා ක්රියාකාරිත්වය පිළිබදව තොරතුරු තේරුම් ගැනීමෙන් පසුව පරීෂකයන් විසින් වෛරසවල ක්රියාකාරිත්වය සවිස්තරාත්මකව තේරුම්ගත් අතර වෛරසවල ප්රජනන චක්රයට බාධාකිරීම සදහා අවශ්යවන රසායනික ද්රව්යය පිළිබදව ද අවබෝධයක් ලබාගත්හ. මේ වන විට ප්රතිවෛරස ඖෂධ දුසිම් ගණනක් වෙළද පොළෙහි ලබාගැනීමට හැකි අතර තව තවත් නව ඖෂධ වර්ග සොයා ගැනීම පිණිස වෛද්ය පර්යේෂකයන් නූතන තාක්ෂණ දැනුම වඩාත් යුහුසුළුව ප්රයෝජනයට ගනිති.
ශ්රී ලංකාවේ මැලේරියා තත්වය
ශ්රී ලංකාවේ මැලේරියාව තුරන් කිරීම වසර 80 ක් තුළ මහජන සෞඛ්ය සාර්ථකත්වයේ කතාවකි. මෙම ජීවිතයට තර්ජනයක් වන රෝගය සමඟ ඇති වූ අසාමාන්ය සටනකින් පසු, 2016 සැප්තැම්බර් මාසයේදී මැලේරියාව තුරන් කිරීම සම්බන්ධයෙන් ලෝක සෞඛ්ය සංවිධානයේ සහතිකය ශ්රී ලංකාවට ලැබුණි.
“1935 දී ශ්රී ලංකාවේ වඩාත් විනාශකාරී පුපුරා යාමේ උච්චතම අවස්ථාවේ දී, මැලේරියා රෝගීන් මිලියන 1.5 කට අධික සංඛ්යාවක් වාර්තා වූ අතර, එහි ප්රතිඵලයක් ලෙස 80 000 ක් මිය ගියහ. මේවා විශ්මය ජනක සංඛ්යාලේඛන වන අතර, විශේෂයෙන් එකල ශ්රී ලංකාවේ ජනගහනය මිලියන 6 ක් පමණ වූ බව ඔබ සලකන විට, ”ශ්රී ලංකාවේ ලෝක සෞඛ්ය සංවිධානයේ නියෝජිත ආචාර්ය ජේකොබ් කුමාරසන් මහතා පැවසීය.
ලෝක සෞඛ්ය සංවිධානයේ ගෝලීය මැලේරියා තුරන් කිරීමේ වැඩසටහන 1955 දී දියත් කිරීමෙන් අනතුරුව, ශ්රී ලංකාව 1957 දී තමන්ගේම මැලේරියා තුරන් කිරීමේ උපාය මාර්ගයක් දියත් කළ අතර එය බොහෝ දුරට සාර්ථක විය.
“ශ්රී ලංකාව මැලේරියාව තුරන් කිරීමට ඉතා ආසන්න විය. 1963 දී මුළු වසර පුරාම අනාවරණය වී ඇත්තේ රෝගීන් 17 ක් පමණි. ශ්රී ලංකාවේ මෙතෙක් වාර්තා වූ අඩුම රෝග බර මෙයයි. නමුත් මැලේරියා වැඩසටහනේ ඇදහිය නොහැකි සාර්ථකත්වයේ ප්රතිඵලයක් ලෙස දේශපාලන හා මූල්යමය ආධාර රැල්ලට ලක්විය. ”වෛද්ය කුමාරසන් මහතා පැවසීය. කෙටි කාලයක් තුළ මැලේරියාව වේගයෙන් හා මාරාන්තික ලෙස නැවත පැමිණියේය. 1970 වන විට මැලේරියා රෝගීන් සංඛ්යාව මිලියනය දක්වා ඉහළ ගිය අතර මැලේරියා මර්දන ව්යාපාරයේ (AMC) පාලන උත්සාහයන් තීව්ර කර තිබියදීත් නැතිවූ භූමිය නැවත ලබා ගැනීමට තවත් දශක පහක් ගතවිය.
AMC සෞඛ්ය සේවකයින් මෙම ක්රියාවලියට තීරණාත්මක වූ අතර බොහෝ විට ආසාදිත මදුරුවන් පිළිබඳව අධ්යයනය කිරීම සඳහා ඉහළ අවදානම් සහිත ප්රදේශවලට ගමන් කිරීමෙන් ඔවුන්ගේ සෞඛ්යය හා ආරක්ෂාව අවදානමට ලක් විය.
“මැලේරියා රෝගයක් පිළිබඳව අප දැනගත්තේ නම්, අපි රෝගියාගේ නිවස සොයාගෙන ආසාදිත මදුරුවන් අවට ප්රදේශවල කොටු කර ගනිමු. අපට දින 39 ක්, සමහර විට සති ගණන් කැලෑවක ගමන් කළ නොහැකි මාර්ග නොමැතිව ගත කිරීමට සිදුවිය. ”කීට විද්යා සහායක දයා විදානපතිරාන මහතා වසර 39 ක් මැලේරියා මර්දන ව්යාපාරය සමඟ වැඩ කළේය.
“අපි මදුරුවන් සඳහා උගුල් අටවන්නෙමු. නමුත් සමහර විට අපි ඇමක් විය. අපට බොහෝ විට උණ වැළඳී ඇත, සමහර විට අපට මැලේරියාවද ඇතිවිය. ”විදානපතිරාන මහතා පැහැදිලි කළේය.
1990 දශකය තුළ, මැලේරියා මර්දන ව්යාපාරය ඔවුන්ගේ උපාය නැවත මතක් කර, මදුරු පාලනයේ සිට පරපෝෂිත පාලනය දක්වා ගමන් කළේය. “අපි වෙනත් රටවලට වෙනස් වන්නේ එලෙසයි. අප මැලේරියාවෙන් මිදුනේ දෛශිකය නොව පරපෝෂිතයා තුරන් කිරීමෙනි. මුල් රෝග විනිශ්චය, ක්ෂණික ප්රතිකාර, දැඩි රෝග නිරීක්ෂණ, කීට විද්යා සමීක්ෂණ, සෞඛ්ය අධ්යාපනය, දැඩි ප්රජා සහභාගීත්වය සහ පර්යේෂණ යන කරුණු සියල්ලම ඉතා සම්බන්ධීකරණ ආකාරයකින් අපි අවධානය යොමු කර ඇත්තෙමු. ” යනුවෙන් මැලේරියා මර්දන ව්යාපාරය හි හිටපු අධ්යක්ෂ වෛද්ය රිසින්ත ප්රේමරත්න මහතා පැවසීය. ලෝක සෞඛ්ය සංවිධානය වැනි ප්රධාන හවුල්කරුවන්ගේ වැඩි දියුණු කළ සහයෝගය සමඟ උපාය මාර්ග මාරුවීම මැලේරියාව තුරන් කිරීමේ අරගලයේ තවදුරටත් සාර්ථක වීමට හේතු විය. “අපගේ සංවර්ධනය හා ප්රගතිය පුරාවටම ලෝක සෞඛ්ය සංවිධානය අපගේ හවුල්කරුවා වී ඇති අතර, අපගේ උපාය මාර්ග සඳහා විශාල දායකත්වයක් ලබා දීම, තාක්ෂණික උපදෙස් හා පුහුණුව ලබා දීම සහ මැලේරියා මූලාරම්භයන් පසුබෑමට සහාය වීම. අපගේ හවුල්කරුවන් වන ඒඩ්ස්, ක්ෂය රෝගය සහ මැලේරියාවට එරෙහි ගෝලීය අරමුදල (GFATM) වෙතින් අපට විශාල සහයෝගයක් ලැබී තිබේ. ”වෛද්ය රිසින්ත පිළිගත්තේය.
2008 වන විට රට තුළ වසරකට මැලේරියා රෝගීන් 1000 කටත් වඩා අඩු සංඛ්යාවක් වාර්තා වී ඇති අතර එමඟින් ශ්රී ලංකාව තුරන් කිරීමේ ඉලක්කය සපුරා ගැනීමට හැකි විය. අවසන් වරට ශ්රී ලංකාව තුලදී පුද්ගල යෙකු හට මැලේරියාව වැළඳී ඇත්තේ 2012 ඔක්තෝම්බර් මාසයේදීය. ස්වදේශික මැලේරියා රෝගීන් ශුන්යව පවත්වා ගෙන ගොස් වසර 3 කට පසුව, 2016 දී මැලේරියාව තුරන් කළ බවට ශ්රී ලංකාවට WHO සහතිකය ලැබුණි.
කෙසේ වෙතත් විදේශ රටවලින් පැමිණෙන දෙස් හා විදෙස් මැලේරියා රෝගීන් 50-100 අතර සංඛ්යාවක් තවමත් වාර්ශිකව වාර්තා වේ.
“ශ්රී ලංකාවේ දන්නා ඉතිහාසයේ මීට පෙර කිසි දිනෙක සිදු නොවූ දෙයක් අප අත්කර ගෙන තිබේ. ඒ ගැන අපි ආඩම්බර වෙනවා. ”වෛද්ය රිසින්ත ප්රේමරත්න පැවසීය.
කෙසේ වෙතත්, 1960 ගණන්වල මැලේරියාව නැවත නැගිටීම පිළිබඳ මතකයන් මැලේරියා මර්දනය සඳහා වැඩ කරන සියලු දෙනාගේ මනසෙහි විශාල වශයෙන් රැඳී තිබේ. මැලේරියාව නැවත හඳුන්වාදීම වැළැක්වීම ඉතිහාසය නැවත නැවත සිදුවීම වළක්වා ගැනීම රටට ඇති ඊළඟ විශාල අභියෝගයයි. ශ්රී ලංකාව ආනයනය සමඟ විශාල තර්ජනයක් වන මැලේරියා සම්ප්රේෂණයට ඇති ඉහළ අවදානම සැලකිල්ලට ගෙන ඉහළ මට්ටමේ සුපරීක්ෂාවක් අවශ්ය වේ.
